Achilles Tendinitis/Tendinosis in Brookfield, WI
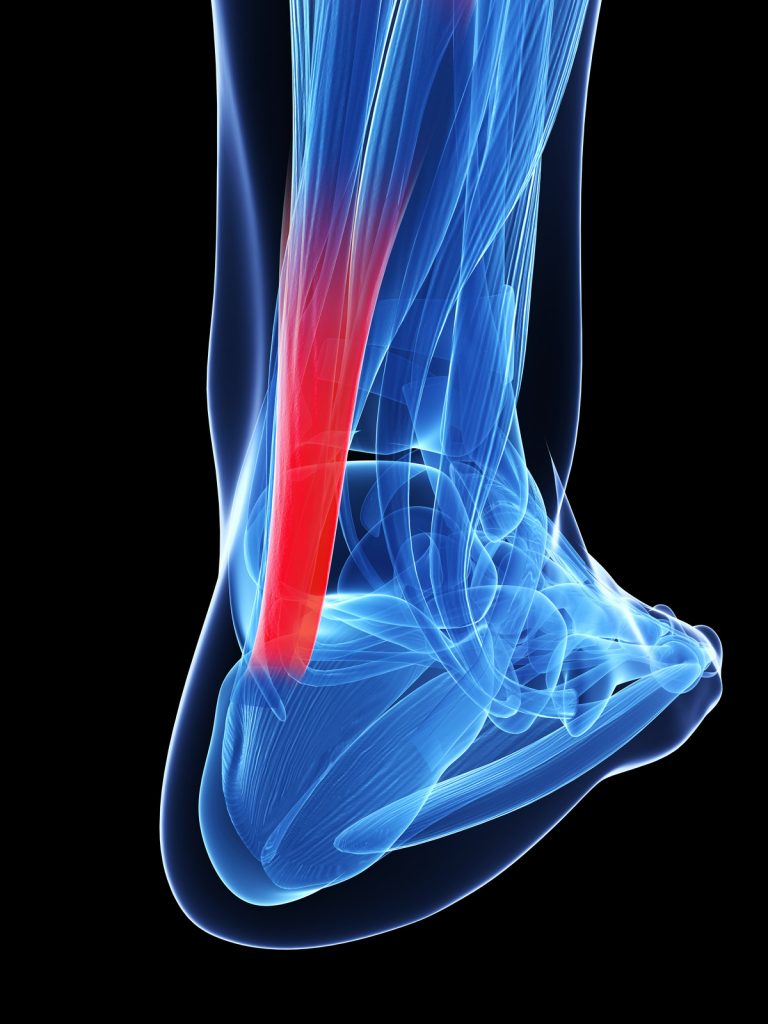
If you have ever experienced Achilles tendonitis, you are well aware of the intense pain that can accompany each step. Even though the Achilles tendon is a large and strong tendon, the amount of force transferred through it while running can easily explain the frequency with which it is injured. The Achilles tendon is the combined tendon of the the two calf muscles: the more superficial gastrocnemius and the deeper soleus. Unlike most tendons, the Achilles actually twists 90 degrees between the calf muscles and its insertion on the heel bone (1). This allows the tendon to act like a rubber band for greater efficiency during running. The Achilles tendon is responsible for taking much of the forces of impact with the ground and transmitting them back into energy during the propulsive period and toe off. This subjects the Achilles tendon to forces up to seven times greater than the body weight of the individual (2)! So while the storage and return of energy inside the Achilles tendon improves running and stride efficiency, the extreme forces stored in the tendon increases the likelihood of injury.
Gradually building running mileage and intensity allows the tendon to adapt to the new stresses. Quickly increasing either mileage or intensity of workouts increases your likelihood of sustaining a tendon or muscle injury.
Symptoms
The symptoms of Achilles tendonitis, or often more appropriately named Achilles tendinosis or tendinopathy, are pretty simple. It is characterized by pain (aching, stiffness, soreness, or tenderness) in the tendon and tenderness, or sometimes intense pain, when the sides of the tendon are squeezed. A “creaky” or “crackling” sensation may also be present with the first few steps after a period of inactivity or when rubbing your fingers along the sides of the tendon. If the condition progresses to degeneration, the tendon may become enlarged and may develop nodules in the area where the tissue is damaged.
Prevention & Self Treatment
There are some simple things that can be done to help avoid Achilles tendinopathies or to treat it quickly at the first signs of symptoms. Easing into exercise routines and warming up properly, as well as regularly stretching and foam rolling the calf muscles after exercise will allow for proper adaptation to work load and muscle recovery after exercise. Wearing the appropriate shoes for your foot type is also very important in preventing running injuries, which is why we work closely with our local running stores to ensure that our patients are being fit for the proper shoes. Periodic preventative treatments such as Graston Technique, Active Release Technique and Dry Needling can also prevent recurrence of this painful condition.
Traditional Treatment
- Immobilization. Immobilization may involve the use of a cast or removable walking boot to reduce forces through the Achilles tendon and promote healing (3).
- Ice. To reduce swelling due to inflammation, apply a bag of ice over a thin towel to the affected area for 20 minutes of each waking hour. Do not put ice directly against the skin.
- Oral medications. Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen, may be helpful in reducing the pain and inflammation in the early stage of the condition.
- Orthotics. For those with over-pronation or gait abnormalities, custom orthotic devices may be prescribed (4).
- Night splints. Night splints help to maintain a stretch in the Achilles tendon during sleep.
Our Integrated Approach
 We carefully analyze your running form and identify areas to correct, improve or strengthen to optimize your form and efficiency, keeping you injury free. Check out more about our Running and Performance Clinic. We also use advanced soft tissue and myofascial release techniques including Graston Technique, Active Release Technique (ART), and trigger point dry needling. We will also prescribe specific stretches and exercises, typically involving eccentric loading activities for the Achilles tendon (5).
We carefully analyze your running form and identify areas to correct, improve or strengthen to optimize your form and efficiency, keeping you injury free. Check out more about our Running and Performance Clinic. We also use advanced soft tissue and myofascial release techniques including Graston Technique, Active Release Technique (ART), and trigger point dry needling. We will also prescribe specific stretches and exercises, typically involving eccentric loading activities for the Achilles tendon (5).
Treatment with Graston, ART, and/or dry needling techniques is often applied to the Achilles tendon, calf muscles, hamstrings and possibly into the muscles of the low back.
Sources:
1. Michaud, Thomas. Human Locomotion: The Conservative Management of Gait-Related Disorders. Newton, MA: Newton Biomechanics, 2011. Print.
2. Mahieu NN, Witvruow E, Stevens V, et al. Intrinsic risk factors for the development of Achilles tendon overuse injuries. Am J Sp Med, 2006;34:226-35.
3. Michaud, Thomas. Foot Orthoses and Other Forms of Conservative Foot Care. Newton, MA: 1997. Print.
4. Johanson M, Allen J, Matsumoto M, et al. Effects of heel lifts on plantarflexor and dorsiflexion activity during gait. Foot Ankle Int, 2010;31:1014-1020.
5. Rees J, Lichtwark G, Wolman R, et al. The mechanism for efficacy of eccentric loading an Achilles tendon injury: an in vivo study in humans. Rheumatology, 2008;47:1493-1497.
 262-373-9168
262-373-9168





 Schedule an Appointment now
Schedule an Appointment now