Plantar Fasciitis in Brookfield, WI
Plantar Fasciitis can be an extremely painful condition, which is caused by inflammation and swelling of the plantar fascia or the thick band of connective tissue on the bottom of the foot. It is the most common cause of heel pain in runners, affecting approximately 10 percent of the running community (1). It is often considered an overuse injury, but may more accurately be caused by poor mechanics in the gait cycle (walking or running), excessive body weight, or improper footwear. Some activities that may predispose a person are running, triathlons, improper stretching, or jobs that involve long periods of standing. Tight or stiff Achilles tendons, calf muscles, hamstrings, or weak foot muscles also increase your risk factors (2). While it’s generally accepted that individuals with flat feet or very high arches may be at increased risk of developing foot pain due to changes in the direction of forces on the plantar fascia tissues, research shows that the relationship between the plantar fascia and flexor digitorum brevis (FDB – or the muscle that flexes the toes) plays a much larger role than arch height (3).
Runners and Plantar Fasciitis
Runners routinely expose the plantar fascia to up to seven times their body weight during the push-off phase. Because of that force, when tension in the plantar fascia gets too high the FDB tenses to distribute pressure away from the overworked plantar fascia. Research evaluating risk-factors for plantar fasciitis showed that the best predictor for future plantar fasciitis development is the speed in which the toes move upward during the propulsive period, not the height of the arch. When the FDB is weak, this upward movement occurs earlier and more quickly (4, 5).
Plantar Fasciitis Symptoms
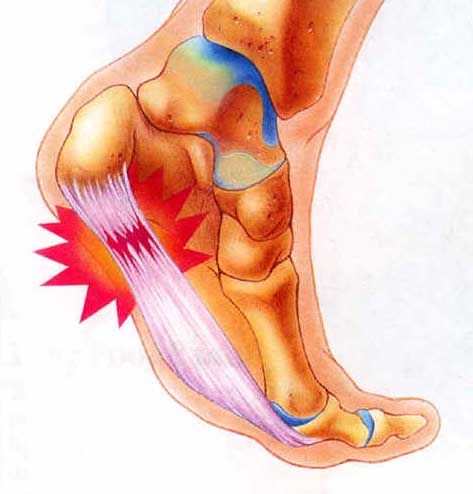
People with plantar fasciitis often complain of pain along the arch of the foot and at the heel. Pain can be excruciating during the first steps after getting out of bed in the morning or after sitting or standing for long periods of time. The plantar fascia, which assists in supporting the arch of the foot, becomes irritated and inflamed when pressure with repetitive movements (walking or running) causes micro-tearing in these tissues. One of the body’s healing responses to this injury is to create scar tissue. This scar tissue is not flexible or elastic and can further complicate the problem by putting further mechanical strain on other areas of the foot, creating a vicious cycle of increasing scar tissue and re-injury (6). Plantar fasciitis can become a chronic injury, often termed plantar fasciosis at this point because there is minimal inflammation. Plantar fasciosis is often characterized by extensive scar tissue that restricts movement due to loss of blood flow to the area. It is very difficult to treat and can take up to two years to completely heal.
Prevention & Self Treatment
There are many things that can be done to help avoid this painful condition or treat it quickly at the first signs of symptoms. Wearing the appropriate shoes for your foot type is very important in preventing plantar fasciitis. We work closely with Performance Running Outfitters to ensure that our patients are being fit for the proper shoes, whether it’s a neutral, stability or motion control shoe. Just as you should stretch and foam roll the muscles in your legs frequently, the same holds true for the muscles and connective tissue in your feet. Whether you choose a tennis ball, golf ball, or water bottle, stretching and rolling the soft tissues in the bottom of your feet will keep those tissues functioning properly and pain-free (7). Periodic preventative treatments such as Graston Technique, Active Release Technique and Dry Needling can also prevent recurrence of this painful condition. Since plantar fasciitis is generally a chronic problem, prevention is an important part of treatment.
Traditional Treatment of Plantar Fasciitis
Common treatments used to alleviate pain and aid in the healing of plantar fasciitis are rest, ice, orthotics, splints such as the Strassburg sock or a rigid orthopedic boot, non-steroidal anti-inflammatories, and physical therapy exercises.
Graston Technique and Active Release Technique (ART)
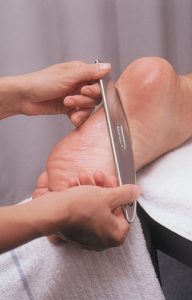 The primary cause of the pain in plantar fasciitis and plantar fasciosis is repeated micro-tearing of the fascia followed by scar tissue formations and adhesions. Traditional treatments alone or together may only minimally reduce the pain and do little to prevent recurrence.
The primary cause of the pain in plantar fasciitis and plantar fasciosis is repeated micro-tearing of the fascia followed by scar tissue formations and adhesions. Traditional treatments alone or together may only minimally reduce the pain and do little to prevent recurrence.
The primary goals of a practitioner using Graston Technique and ART for Plantar Fasciitis:
- Aid in the disruption/breakdown of the adhesions
- Increase normal tissue flexibility, movement and comfort
- Aim to restore full flexibility, balance and stability
Treatment with Graston and ART techniques is often applied to the plantar fascia, calf muscles, hamstrings and other muscles of the foot. The treatment is complemented with specific foot stretches strengthening exercises (8). Most patients report a positive response within 4-6 treatments.
Sources
1. DeMaio M, Paine R, Mangine RE, Drez DJr. Plantar fasciitis. Orthopedics 1993; 16:1153-1163.
2. Michaud, Thomas. Foot Orthoses and Other Forms of Conservative Foot Care. Newton, MA: 1997. Print.
3. Michaud, TC. New techniques for treating plantar fasciitis. Published Jun. 6, 2014, Competitor.com
4. Wearing S, Smeathers J, Yates B, et al. Sagittal movement of the medial longitudinal arch is unchanged in plantar fasciitis. Med Sci Sports Exerc. 2004;36:1761- 1767.
5. Menz H, Zammit G, Munteanu S, Scott G. Plantarflexion strength of the toes: age and gender differences and evaluation of a clinical screening test. Foot Ankle Int. 2006; 27:1103-1108.
6. Michaud, Thomas. Human Locomotion: The Conservative Management of Gait-Related Disorders. Newton, MA: Newton Biomechanics, 2011. Print.
7. DiGiovanni B, Nawoczenski D, Lintal M, et al. Tissue-specific plantar fascia-stretching exercise enhances outcomes in patients with chronic heel pain. A prospective, randomized study. J Bone Joint Surg. 2003;85-A:1270–1277.
8. Renan-Ordine R, Alburquerque-Sendin F, Rodrigues De Souza D, et al. Effectiveness of myofascial trigger point manual therapy combined with a self-stretching protocol for the management of plantar heel pain: a randomized controlled trial. J Orthop Sports Phys Ther. 2011;41:43.
 262-373-9168
262-373-9168





 Schedule an Appointment now
Schedule an Appointment now